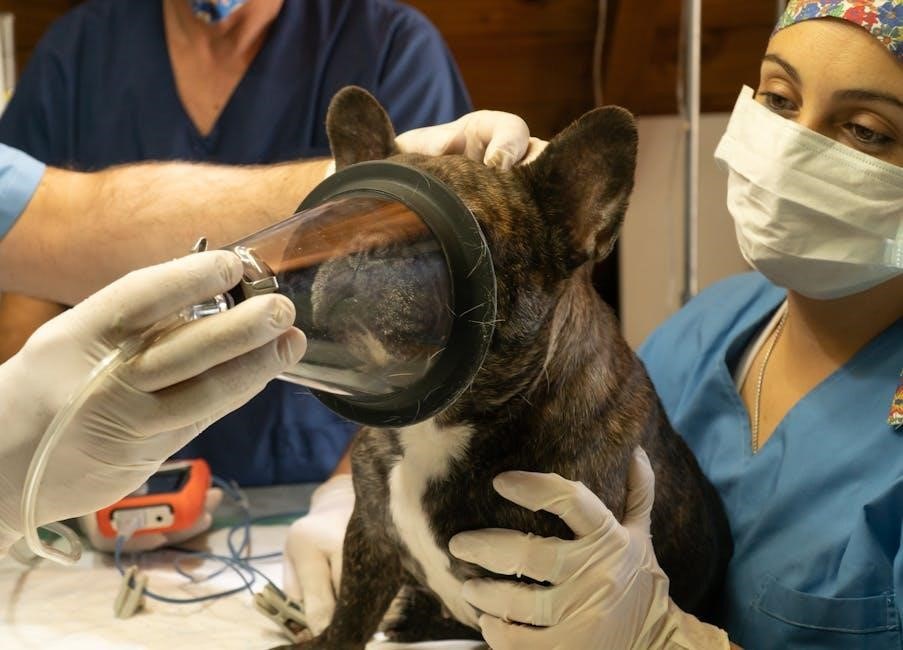
Recent DAHD guidelines address a critical shortage of blood products, prompting vets to seek more emergency animal donors for vital transfusions.
What is Plasma and Why Use It?
Plasma, the liquid component of blood, contains vital proteins – including clotting factors and antibodies – crucial for maintaining physiological balance. Veterinary plasma transfusions are frequently employed when patients experience significant protein deficiencies or compromised immune systems.
Specifically, it’s invaluable in cases of hypovolemia, aiding in volume expansion, and addressing coagulation disorders. Animals recovering from trauma, or those suffering from protein-losing diseases, often benefit greatly from plasma support. The recent push for donor registration highlights its increasing necessity.
Types of Plasma Available for Veterinary Use
Currently, fresh frozen plasma (FFP) is the most commonly utilized type in veterinary medicine, preserving all coagulation factors and proteins. While autologous plasma – collected from the patient themselves – offers ideal compatibility, it’s not always feasible.
Lyophilized plasma products represent a promising future trend, offering extended shelf life and easier storage. However, their widespread availability is still developing. Standard plasma collection relies on anticoagulants to prevent clotting during processing, ensuring its therapeutic efficacy when administered to recipient animals.

Indications for Plasma Transfusion
Plasma transfusions are crucial for addressing hypovolemia, coagulation deficits, and protein loss, frequently seen in trauma cases and various systemic diseases.
Hypovolemic Shock and Plasma Expansion
Hypovolemic shock, often resulting from hemorrhage or severe fluid loss, demands rapid plasma expansion to restore circulating volume. Plasma’s high protein content, particularly albumin, effectively increases oncotic pressure, drawing fluid into the vasculature. This is especially vital in cases of road trauma or significant blood loss where crystalloids alone may be insufficient.
Plasma provides not only volume but also essential clotting factors, aiding in hemostasis alongside volume resuscitation. Its use can bridge the gap until definitive hemorrhage control is achieved or whole blood products become available, improving patient outcomes significantly. Careful monitoring of response is essential.
Coagulation Disorders and Plasma’s Role
Plasma is a cornerstone in managing coagulation disorders due to its rich supply of clotting factors. Conditions like disseminated intravascular coagulation (DIC), liver disease-induced factor deficiencies, and inherited clotting factor deficiencies benefit greatly from plasma transfusion. It rapidly replenishes these vital components, supporting the coagulation cascade.
However, plasma isn’t a universal fix. The specific deficiency must be considered, and monitoring of coagulation parameters (PT, aPTT) post-transfusion is crucial to assess efficacy. In some cases, specific factor concentrates may be preferred for targeted therapy, but plasma remains a valuable, readily available option.
Protein Lossing Nephropathy/Enteropathy
Plasma transfusions offer critical support for patients suffering from protein-losing nephropathy (PLN) or enteropathy (PLE). These conditions result in substantial loss of plasma proteins, particularly albumin, leading to hypoalbuminemia and subsequent edema and ascites. Plasma provides a temporary source of these essential proteins, helping to restore oncotic pressure.
While not curative, plasma can improve clinical signs and provide supportive care while addressing the underlying cause of protein loss. Frequent transfusions may be necessary, and monitoring albumin levels is vital to gauge response and adjust therapy accordingly.
Immune-Mediated Diseases
Plasma transfusions can be a valuable adjunct therapy in managing immune-mediated diseases in veterinary medicine. Specifically, plasma contains immunoglobulins that can temporarily modulate the immune system, offering benefit in conditions like immune-mediated hemolytic anemia (IMHA) or thrombocytopenia (ITP).
The transfused antibodies can help neutralize autoantibodies or provide passive immunity, reducing disease severity. However, plasma is typically used as a bridge to definitive immunosuppressive therapy, not as a standalone treatment. Careful monitoring for transfusion reactions is crucial in these sensitive patients.
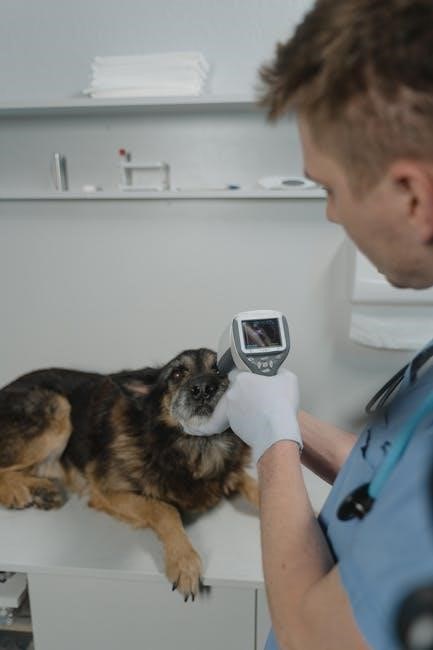
Donor Selection and Collection
Healthy animals donating every four to eight weeks are crucial, with cats often requiring sedation during collection to ensure a safe and efficient process.
Ideal Donor Characteristics
Selecting appropriate donors is paramount for safe and effective plasma transfusions. Ideal candidates possess a robust health history, demonstrating freedom from infectious diseases and prior blood product exposure. They should exhibit normal physiological parameters – temperature, pulse, respiration – and maintain a consistent body weight.
Donors must be regularly screened for common pathogens and possess appropriate temperament for the collection procedure. Age and parity are also considerations, with mature, multiparous animals often preferred. A complete physical examination confirms overall health, ensuring the donor can tolerate the donation process without adverse effects.
Plasma Collection Techniques
Several techniques facilitate plasma collection, prioritizing donor safety and product quality. Phlebotomy, utilizing a sterile collection set, is a common method, drawing whole blood into a collection bag containing an anticoagulant. Centrifugation then separates plasma from cellular components.
Automated collection systems are increasingly employed, streamlining the process and minimizing donor handling time. Cats often require sedation during collection to ensure comfort and cooperation. Careful monitoring of the donor throughout the procedure is crucial, observing for any signs of distress or adverse reactions.
Anticoagulant Used in Plasma Collection
Citrate Phosphate Dextrose Adenine (CPDA-A) is the standard anticoagulant used in veterinary plasma collection. This solution effectively prevents blood coagulation by chelating calcium ions, essential for the clotting cascade. CPDA-A also provides nutrients to support cell viability during storage, preserving plasma quality.
The correct ratio of CPDA-A to blood is critical for optimal anticoagulation and minimizing adverse effects. Alternative anticoagulants exist, but CPDA-A remains the most widely recommended due to its efficacy and established safety profile in veterinary medicine. Proper handling and storage of CPDA-A are also essential.

Plasma Processing and Storage
Plasma requires careful centrifugation for separation, followed by freezing and proper thawing procedures to maintain its therapeutic efficacy and ensure quality control.
Centrifugation and Separation
Effective plasma processing begins with centrifugation, a crucial step to separate plasma from cellular components. This typically involves a two-stage spin – an initial slow spin to separate red blood cells, followed by a higher-speed spin to isolate the buffy coat (white blood cells and platelets) and ultimately, the clear plasma.
Care must be taken to avoid hemolysis during this process, as damaged red blood cells release substances that can compromise plasma quality. Following centrifugation, the plasma is carefully removed, ensuring minimal contamination from other blood components. Proper technique and equipment maintenance are vital for optimal separation.
Freezing and Thawing Procedures
Proper freezing is essential for long-term plasma preservation. Plasma should be rapidly frozen to -80°C or lower to minimize ice crystal formation, which can damage proteins. Controlled-rate freezing is often preferred.
Thawing must be performed quickly, ideally in a 37°C water bath, with gentle agitation. Avoid prolonged thawing at room temperature. Once thawed, plasma should be used immediately and not refrozen. Careful adherence to these procedures maintains plasma’s therapeutic efficacy and prevents degradation of vital clotting factors and proteins.
Storage Duration and Quality Control
Frozen plasma can be stored for up to one year, though some institutions extend this to two years with rigorous quality control. Regular monitoring of clotting factor activity is crucial to ensure efficacy.
Visual inspection for hemolysis or particulate matter is also vital before administration. Accurate record-keeping of collection and storage dates is paramount. Hospitals should establish SOPs for routine quality checks, including bacterial contamination screening, to guarantee patient safety and maintain plasma product integrity throughout its storage lifespan.

Administration Techniques
Plasma volume calculations are essential, typically administered intravenously. Careful monitoring during transfusion is critical to detect and manage any potential adverse reactions promptly.
Calculating Plasma Volume
Determining the appropriate plasma volume for transfusion requires careful consideration of the patient’s body weight and the severity of their condition. A common starting point is 5-10 ml/kg body weight, but this can be adjusted based on the clinical response and ongoing monitoring.
Factors influencing the volume include the degree of hypovolemia, protein loss, or coagulation factor deficiency. It’s crucial to reassess the patient frequently after initial administration, evaluating parameters like packed cell volume (PCV), total protein, and clinical signs.
Smaller, incremental doses are often preferred, especially in critically ill patients, to minimize the risk of circulatory overload. Accurate weight estimation is paramount for precise dosage calculations.
Intravenous Administration Protocols
Plasma should be administered slowly intravenously, ideally through a dedicated intravenous catheter, using a blood warmer to prevent hypothermia, especially with larger volumes. A typical infusion rate is 1-5 ml/kg/hour, closely monitored for adverse reactions.
Pre-transfusion vital signs (temperature, pulse, respiration rate, blood pressure) are essential baseline data. During administration, continuous monitoring is critical, observing for signs of allergic reaction or circulatory overload.
Use of a filter (180-micron) is recommended to remove any potential clots or debris. Frequent reassessment of the patient’s clinical status guides adjustments to the infusion rate.
Monitoring During Transfusion
Vigilant monitoring is paramount during plasma transfusion, starting before initiation with baseline vital signs – temperature, pulse, respiration, and blood pressure. Continuously observe for early signs of reaction: fever, urticaria, facial edema, or dyspnea.
Assess the patient frequently (every 5-15 minutes initially) for any adverse effects. Auscultate lung sounds to detect potential pulmonary edema, indicative of circulatory overload.
Monitor mucous membrane color and capillary refill time as indicators of perfusion. Document all observations meticulously, and be prepared to stop the transfusion immediately if a reaction occurs.
Potential Complications of Plasma Transfusion
Transfusion reactions, including anaphylaxis and febrile responses, are possible, alongside risks like TRALI and circulatory overload, demanding careful monitoring.
Transfusion Reactions (Anaphylaxis, Febrile Reactions)
Plasma transfusions, while life-saving, carry the risk of adverse reactions. Anaphylaxis, a severe and potentially fatal allergic reaction, requires immediate intervention with epinephrine and supportive care. More commonly, febrile non-hemolytic transfusion reactions occur, presenting as fever and chills, often managed with antipyretics.
Careful monitoring is crucial during and after transfusion. Observing for signs like hives, facial swelling, difficulty breathing, or changes in vital signs is paramount. Pre-medication with antihistamines or corticosteroids may mitigate milder reactions. Prompt recognition and appropriate treatment are essential for patient safety.
Transfusion-Related Acute Lung Injury (TRALI)
TRALI represents a serious, though rare, complication of plasma transfusion. It’s characterized by acute respiratory distress, pulmonary edema, and hypoxemia, typically developing within six hours of transfusion. The underlying cause involves donor antibodies reacting with recipient leukocytes, leading to lung inflammation.
Diagnosis relies on clinical signs and ruling out other causes of acute lung injury. Supportive care, including oxygen therapy and mechanical ventilation, is critical. Prevention focuses on careful donor selection and, ideally, leukocyte-reduced blood products. Vigilant monitoring for respiratory distress is paramount during and post-transfusion.
Circulatory Overload
Circulatory overload is a significant risk, particularly in patients with compromised cardiac function. Rapid plasma infusion can exceed the circulatory system’s capacity, leading to pulmonary edema and congestive heart failure. Signs include increased respiratory rate, coughing, and crackles upon auscultation.
Careful calculation of plasma volume and slow administration rates are crucial preventative measures. Monitoring vital signs, especially respiratory parameters, throughout the transfusion is essential. Diuretics may be administered proactively or to manage existing overload. Pre-existing conditions like renal or cardiac disease heighten susceptibility.

Guidelines and Standard Operating Procedures (SOPs)
The DAHD recently released guidelines and SOPs to address blood product shortages and standardize plasma transfusion practices within veterinary medicine.
DAHD Guidelines for Blood Product Use
The Department of Animal Husbandry and Dairying (DAHD) guidelines are crucial for ensuring safe and effective blood product administration in veterinary practice. These guidelines, released under the Ministry of Fisheries, Animal Husbandry & Dairying, aim to standardize procedures nationwide. They address the growing concern of blood product shortages, urging increased pet registration for emergency donation programs.
The DAHD emphasizes the importance of proper donor selection, collection techniques, and storage protocols to maintain plasma quality. Furthermore, the guidelines promote adherence to hospital-specific Standard Operating Procedures (SOPs) alongside national recommendations, fostering a consistent approach to plasma therapy across India.
Hospital-Specific SOPs for Plasma Transfusion
Each veterinary hospital must develop detailed Standard Operating Procedures (SOPs) supplementing the national DAHD guidelines. These SOPs should outline specific protocols for plasma transfusion, encompassing donor eligibility criteria, collection methods, and rigorous quality control measures.
Detailed documentation is essential, including plasma processing, storage, and administration techniques. SOPs must also address potential complications like transfusion reactions and circulatory overload, outlining immediate response protocols. Regular staff training on these SOPs ensures consistent, safe, and effective plasma therapy, tailored to the hospital’s resources and patient population.
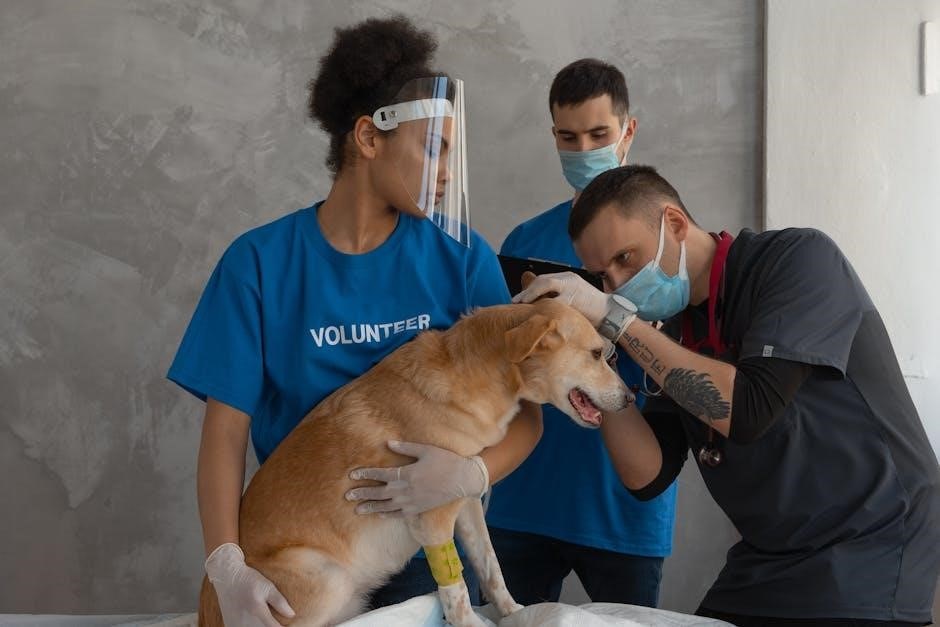
Blood Typing and Crossmatching
Blood typing is crucial, though emergency protocols exist when immediate transfusion is needed, prioritizing patient survival despite lacking complete typing data.
Importance of Blood Typing
Accurate blood typing is paramount in veterinary transfusion medicine to minimize the risk of adverse reactions. While universal donors exist, identifying a patient’s blood type – particularly DEA 1.1 and DEA 7 – significantly improves transfusion safety. Mismatched transfusions can lead to severe hemolytic crises, characterized by rapid red blood cell destruction and potentially fatal consequences.
Although emergency transfusion protocols allow for type-unmatched plasma administration in life-threatening situations, proactive typing reduces these risks. Establishing a robust blood typing program within veterinary practices and utilizing readily available testing kits are essential components of responsible plasma and blood product usage.
Crossmatching Procedures
Crossmatching involves mixing the recipient’s serum with the donor’s red blood cells to detect incompatible antibodies. A major crossmatch assesses the recipient’s reaction to donor red cells, while a minor crossmatch examines the donor’s reaction to recipient serum. Though not always feasible due to time constraints, crossmatching significantly enhances transfusion safety beyond blood typing alone.
Visual assessment for agglutination (clumping) or hemolysis (red cell breakdown) indicates incompatibility. Positive results contraindicate transfusion. However, negative crossmatches don’t guarantee complete compatibility, emphasizing the importance of careful patient monitoring during and after plasma administration.
Emergency Transfusion Protocols (When Typing is Not Possible)
In life-threatening emergencies, delaying transfusion for typing/crossmatching is unacceptable. Universal donor plasma (typically type AB) can be used initially, minimizing immediate risks. However, this is a temporary measure. Rapid blood typing kits, if available, should be utilized as quickly as possible to identify the recipient’s blood type.
Careful observation for adverse reactions is paramount during emergency transfusions. Once stable, definitive typing and crossmatching must be performed to transition to type-specific plasma. Documentation of the emergency protocol and rationale is crucial for medical records.
Future Trends in Plasma Therapy
Lyophilized plasma products and autologous transfusions represent promising advancements, potentially addressing current shortages and improving patient safety in veterinary medicine.
Lyophilized Plasma Products
The development of lyophilized (freeze-dried) plasma offers significant logistical advantages over frozen plasma. Currently, maintaining the cold chain for frozen plasma presents challenges for many veterinary practices, particularly those in remote locations or emergency situations. Lyophilization would create a shelf-stable product, reducing storage concerns and simplifying distribution.
This enhanced stability allows for easier transport and longer storage durations without compromising efficacy. Furthermore, lyophilized plasma could potentially reduce the risk of transmitting infectious agents due to the freeze-drying process. Research and development are ongoing to optimize lyophilization techniques for veterinary plasma, aiming for a cost-effective and readily available alternative.
Autologous Plasma Transfusion
Autologous plasma transfusion, utilizing a patient’s own plasma, represents an ideal solution to eliminate the risks of alloimmunization and transfusion reactions. This approach involves collecting plasma from the animal prior to an anticipated need, such as elective surgery or during a stable period of a chronic illness like protein-losing nephropathy.
The collected plasma is then stored frozen until required. While requiring foresight and a stable patient, autologous transfusion avoids the challenges of donor availability and blood typing. It’s a particularly valuable option for animals with repeated transfusion needs, minimizing long-term complications.